NL Journal of Dentistry and Oral Sciences
(ISSN: 3049-1053)
The Prevalence of MSMT and its Association with Periapical Lesion and Periodontal Bone Loss using Cone-Beam Computed Tomography
Author(s) : Elham Romoozi, Negar Boroumand, Golsa Ketabchi, Parisa Barouti, Habibollah Rahimi, Mohammadreza Molaee, Shahabaldin Nazeri. DOI : 10.71168/NDO.02.01.103
Abstract
Objective: This study aimed to examine the prevalence of Maxillary Sinus Mucosal Thickening (MSMT) and its association with the dental status of the adjacent teeth, including periapical lesions and PBL, using Cone Beam Computed Tomography (CBCT). Materials and Methods: This retrospective study analyzed 322 maxillary sinuses. MSMT was considered pathological if it exceeded 2 mm and was classified as localized or generalized based on the extent of the affected area. The periapical and periodontal status of 1092 posterior teeth were investigated. CBCTPAI was used to investigate the periapical lesion size; the distance from the upper edge of the lesion to the sinus floor was also studied. PBL was evaluated by pattern (horizontal or vertical) and severity. Results: The prevalence of MSMT in all samples was 34.8% (95% CI: 29.5-40.0%). Of these, 73.2% were localized and 26.8% were generalized. There was a significant correlation between periapical lesions and MSMT (P<0.001), as well as between PAL size and MSMT (P0.05). Conclusions: This study used CBCT imaging for its high accuracy and sensitivity compared to two-dimensional radiographs. The results showed that MSMT was not related to age or gender. The presence and size of periapical lesions increased the likelihood of MSMT, while the distance of the lesions from the sinus floor decreased it. The type of MSMT did not depend on the dental condition. The presence, pattern, and severity of PBL did not affect MSMT. Keywords: Maxillary sinus, Cone-beam computed tomography, Periapical Periodontitis, Alveolar bone loss.
Introduction
The maxillary sinus is the largest paranasal sinus, located bilaterally around the nasal cavity and below the orbit [1]. The maxillary sinus floor typically extends from the first premolar to the maxillary tuberosity [2,3].
One of the most common pathological findings of the maxillary sinus is MSMT (MSMT) [4]. Mucosal thickness greater than 1-3 mm is considered pathological [5], and its prevalence has been reported as 35.1%- 66% in various studies [6-11]. In radiographic images, MSMT can be seen as localized or generalized.
MSMT can be caused by odontogenic infections [12,13], which have increased in prevalence in recent decades [14].
The maxillary sinus can be affected by odontogenic infections due to its anatomical relationship with upper jaw teeth [15]. Odontogenic sinus diseases can range from inflammation and localized MSMT to generalized MSMT and maxillary sinusitis [16-18]. Periapical and periodontal infections are among the odontogenic causes of MSMT [16].
To diagnose sinus diseases radiographically, CT[1], CBCT, and MRI[2] can be used [18]. CBCT has lower radiation dose and cost than conventional CT and provides three-dimensional images of craniofacial structures for dental purposes [19,20]. CBCT can detect changes in the maxillary sinus [21] as well as their possible causes, such as the condition of the adjacent teeth [22].
Materials and Methods
CBCT images collection
This study was approved by the IRB of Kashan University of Medical Sciences (IR.KAUMS.MEDNT.REC.1401.077) on July 26, 2022. This retrospective descriptive-analytical study examined CBCT images of patients referred to an oral, maxillofacial radiology center[1] in Kashan City between 2019 and 2021. Most of the CBCTs were taken for radiological evaluation before implant procedures. The inclusion criteria were CBCTs of visitors to a radiology center in Kashan City from August 2019 to October 2021 who were over 18 years old and had at least one posterior maxillary tooth. The exclusion criteria were CBCT images with radiographic signs of tumor or other maxillary sinus disorders (such as polyps, pseudo-cysts, and enteroliths) [11], presence of implants (due to the possibility of sinus changes during surgical procedures), history of ortho-surgery or orthodontic appliances, poor quality or insufficient FOV CBCT images and CBCT images with signs of allergic or acute sinusitis.
CBCT images evaluation
All CBCT images were taken using the Planmeca 3D (Helsinki, Finland) High-resolution device (mA: 6, kVp: 89, FOV: 8x10 cm2) by an experienced radiologist according to the manufacturer’s recommendations. Then, the images were processed by Romex is 3D Dental software.
Maxillary sinus evaluation
By examining the CBCT images from sagittal and coronal views, MSMT was considered pathological if it exceeded 2 mm [23,24] and affected up to two adjacent teeth (localized) or if it exceeded 2 mm and involved the entire sinus floor (generalized) [25]. Also, the maximum thickness of the radiopaque areas to the sinus floor was measured as the maxillary sinus mucosal thickness (Figure 1) [25].
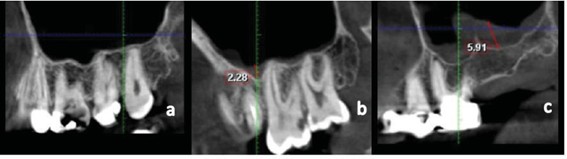
Figure 1. Sagittal views of the maxillary sinus. a. Normal mucosa, b. Localized mucosal thickening generalized mucosal thickening.
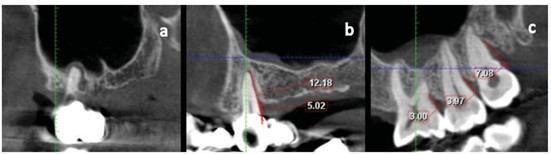
Figure 2. Sagittal views of the maxillary sinus and posterior upper teeth, a. Peri-apical lesion, b. Horizontal bone loss, c. Vertical bone loss.
Dental condition evaluation Peri-apical lesions4
Radiolucency associated with at least one root of a tooth and a diameter of at least 0.5 mm or more than twice the diameter of a healthy periodontal ligament [26] was considered a peri-apical lesion.
An index called CBCTPAI was used to evaluate a tooth’s periapical tissue condition better. This index divides the PAL according to its diameter as follows [27]:
- The periapical bone structure is
- The diameter of the PAL is 5 to 1 mm.
- The diameter of the PAL is 1 to 2
- The diameter of the PAL is 2 to 4
- The diameter of the PAL is 4 to 8
- The diameter of the PAL is more than 8 mm (Figure 2).
Also, the distance from the upper edge of the PAL to the floor of the sinus was measured as follows:
- The distance between the upper edge of the PAL and the maxillary sinus floor is 0 mm or
- The distance from the upper edge of the PAL to the floor of the maxillary sinus is 0 to 2
- The distance from the upper edge of the PAL to the floor of the maxillary sinus is more than 2
Periodontal bone loss5
The pattern of PBL was evaluated as follows:
- Horizontal: This is the most common pattern of bone loss in periodontal diseases, in which the edge of the resorbed bone forms a nearly perpendicular angle with the tooth surface [28].
- Vertical: In this pattern, the edge of the bone forms an acute angle with the tooth surface [28].
Vertical bone loss is classified according to the number of bony walls surrounding the defect. Angular defects may have one, two, or three walls.
The severity of horizontal PBL was assessed based on Phothikhun’s criteria [30] as follows:
(Bone height with a maximum distance of 2 mm below the cementoenamel junction is considered normal; if this distance increases, alveolar bone loss has occurred.)
- Less than 25% bone loss: mild
- 25-50% bone loss: Moderate
- More than 50% bone loss: Severe
Finally, the relationship between the MSMT types and the adjacent teeth’ condition was investigated.
Statistical analysis
The results of this study were analyzed using descriptive statistics (percentage frequency). The chi-square and Fisher’s tests were used to evaluate the relationship between MSMT types and dental conditions. The significance level was considered at P>0.05, and statistical analysis was performed using SPSS statistical software.
Results
In this study, among 322 samples, most of them were from female patients (78.3%). The average age of the samples was 42.2 ± 12.8 years, and the prevalence rate of MSMT in all the samples was 34.8% (29.5-40.0%: 95% CI) (Table 1). We also found that the prevalence rate of different types of MSMT, i.e., localized and generalized thickening, among the samples with MSMT was 73.2% and 26.8%, respectively (Table 2). There was no significant relationship between the prevalence of MSMT and age (Table 3, Figure 3).
| Variable | n | % | 95% Cl |
| Increased Mucosal thickness | 112 | 34.8 | 29.4-75.2 |
| Normal mucosal thickness | 210 | 65.2 | 59.7-82.2 |
| Total | 322 | 100 | - |
Table 1. Prevalence of MSMT.
| Variable | n | % | 95% Cl |
| localized Mucosal thickening | 82 | 73.2 | 64.8-12.7 |
| generalized Mucosal thickening | 30 | 26.8 | 19.3-30.9 |
| Total | 112 | 100 | - |
Table 2. Prevalence of types of MSMT (generalized & localized).
|
Sex |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| Male | 70 | 47 (67.1%) | 23 (32.8%) |
P>0.05 |
| Female | 252 | 163
(64.7%) |
89 (35.3%) | |
| Total | 322 | 210
(65.2%) |
112
(34.8%) |
|
Table 3. Prevalence rate of maxillary sinus mucus thickness increases according to gender.
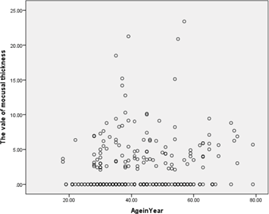 Figure 3. Distribution of MSMT.
Figure 3. Distribution of MSMT.
Among the 322 samples, 125 (38.8%) had at least one tooth with a periapical lesion. We studied the relationship between the PAL and MSMT and found a significant relationship between them (P<0.001) (Table 4). Then, we examined the relationship between the PAL and the type of MSMT (generalized or localized) and found no significant relationship (P>0.05) (Table 5). We also examined the diameter of the PAL using the CBCTPAI [29], and there was a statistically significant relationship between them (P<0.001) (Table 6). Moreover, we measured the distance between the upper edge of the PAL and the floor of the maxillary sinus, and there was a statistically significant relationship between them (P<0.001) (Table 7).
|
Periapical lesion |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| Absence | 197 | 146
(74.1%) |
51 (25.9%) |
P<0.000 |
| Presence | 125 | 64 (51.2%) | 61 (48.8%) | |
| Total | 322 | 210
(65.2%) |
112 (34.8%) | |
Table 4. Relationship between peri-apical lesion and MSMT.
|
Periapical lesion |
Type of Mucosal thickening |
p-value |
|
| localized N (%) | generalized N (%) | ||
| Absence | 36 (70.6%) | 15 (29.4%) |
0.566 |
| Presence | 46 (75.4%) | 15 (24.6%) | |
| Total | 82 (73.2 %) | 30 (26.8%) | |
Table 5. Relationship between peri-apical lesion and types of MSMT.
a:
- There is no peri-apical
- The diameter of the peri-apical lesion is 5 to 1 mm.
- The diameter of the peri-apical lesion is 1 to 2
- The diameter of the peri-apical lesion is 2 to 4
- The diameter of the peri-apical lesion is 4 to 8
- The diameter of the peri-apical lesion is more than 8
| Diameter of peri-apical lesion according to CBCTPAIa index |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| 0 | 197 | 146 (74.1%) | 51 (25.9%) |
P<0.000 |
| 1 | 12 | 7 (58.3%) | 5 (41.7%) | |
| 2 | 42 | 28 (66.7%) | 14 (33.3%) | |
| 3 | 45 | 21 (46.7%) | 24 (53.3%) | |
| 4 | 25 | 8 (32%) | 17 (68%) | |
| 5 | 1 | 0 (0%) | 1 (100%) | |
| Total | 322 | 210 (65.2%) | 112 (34.8%) | |
Table 6. The relationship between the peri-apical lesion diameters according to CBCTPAI. Index and the MSMT.
| Distance between the upper edge of the peri-apical lesion and maxillary sinus floor (millimeters) |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| ≥0 | 21 | 8 (38.1%) | 13 (61.9%) |
P<0.000 |
| 0< <2 | 57 | 25 (43.9%) | 32 (56.1%) | |
| ≤2 | 47 | 31 (66%) | 16 (34%) | |
| Total | 125 | 210 (65.2%) | 112 (34.8%) | |
Table 7. The relationship between the distance of the upper edge of the peri-apical lesion in millimeters and the MSMT.
Among the 322 samples, 138 (42.8%) had at least one tooth with PBL. The prevalence of samples with PBL according to the pattern of bone loss, i.e., horizontal or vertical, was 79.7% and 20.3%, respectively. In this study, we not only examined the samples for the presence of MSMT and PBL but also for the type of MSMT (localized or generalized), the pattern of PBL (horizontal or vertical bone loss), and the severity of horizontal PBL (mild, moderate or severe). We found no statistically significant relationship between them (P>0.05) (Table 8-11).
|
PBL |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| Absence | 184 | 127 (69%) | 57 (31%) |
0.098 |
| Presence | 138 | 83 (60.1%) | 55 (39.9%) | |
| Total | 322 | 210 (65.2%) | 112 (34.8%) | |
Table 8. Relationship between PBL and the MSMT.
|
PBL |
Type of Mucosal thickening |
p-value |
|
| localized N (%) | generalized N (%) | ||
| Absence | 45 (78.9%) | 12 (21.1%) |
0.163 |
| Presence | 37 (67.3%) | 18 (32.7%) | |
| Total | 82 (73.2 %) | 30 (26.8%) | |
Table 9. Relationship between PBL and type of the MSMT.
|
PBL |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| horizontal | 110 | 70 (63.6%) | 40 (36.4%) |
0.097 |
| vertical | 28 | 13 (46.4%) | 15 (53.6%) | |
| Total | 138 | 83 (60.1%) | 55 (39.9%) | |
Table 10. Relationship between type of PBL and the MSMT.
|
Horizontal PBL |
n |
Mucosal thickening |
p-value |
|
| Absence N (%) | Presence N (%) | |||
| mild | 98 | 61 (62.2%) | 37 (37.8%) |
0.566 |
| moderate/severe | 12 | 9 (75%) | 3 (25%) | |
| Total | 110 | 70 (63.6%) | 40 (36.4%) | |
Table 11. Relationship between severity of horizontal PBL and MSMT.
Discussion
CBCT imaging allows for three-dimensional analysis of jaw and facial structures with high-resolution images. This technique is more sensitive and accurate than two-dimensional radiographs. It can simultaneously and precisely evaluate maxillary sinuses [13,14], teeth, and adjacent tissues in coronal, sagittal, and axial dimensions. Therefore, this study used CBCT imaging because of its wide application and high accuracy and sensitivity compared to two- dimensional radiographs. However, CBCT imaging may overestimate the thickness of the Schneiderian membrane compared to histological measurements [29]. In this study, we chose a 2 mm thickness of maxillary sinus mucosa as the pathological limit, even though previous studies suggested a 1-3 mm range.
This study examined 195 patients, 322 maxillary sinuses, and 1092 posterior permanent teeth (from the first premolar to the third molar).
The association between the peri-apical lesion and MSMT
We found a significant relationship between having a PAL and having MSMT (P<0.001). Hong et al.’s study [30] and Nascimento et al.’s study [25] also found a significant relationship between these two factors. However, Phothikhun et al.’s study [31] found no significant relationship between them. This could be because Phothikhun et al.’s study had a lower prevalence of PAL (7.8 percent) and a lower diagnostic criterion of MSMT (1 mm) than this study (2 mm).
We also investigated the relationship between the PAL and the type of MSMT (generalized or localized), and we did not find a significant relationship between them (P>0.05). Nascimento et al.’s study [25] concluded that the PAL could cause a “localized” MSMT. Other studies did not differentiate between the types of MSMT.
We used the CBCTPAI index [27] to examine the diameter of the PAL in this study, and we observed that the prevalence of MSMT increased almost continuously with the increase in lesion diameter. We also found that the prevalence of MSMT increased significantly with the decrease in this distance in millimeters. Therefore, we expect that the prevalence of MSMT is related to the increase in lesion diameter and the reduction in the length from its upper edge to the sinus floor. The results of our study were consistent with the investigations of Nance et al. [8] and Nascimento et al. [25].
The association between PBL and MSMT
In this study, no significant relationship was found between PBL and MSMT. However, Sheikhi et al. [32] and Shahidi et al. [33] reported that PBL is significantly related to increased maxillary sinus mucosa thickness. Nascimento et al. [25] reported that mild and moderate/severe bone loss increased the prevalence of “generalized” mucosal thickening. Phothikhun et al. [31] observed a significant link between the severe type of PBL and the increase in MSMT.
The presence of bone loss due to the decrease in the height of the bone barrier to the maxillary sinus floor can facilitate the penetration of odontogenic infection into the maxillary sinus space [8, 34-36].
Conclusion
However, bone loss cannot increase mucosa thickness without active infection (bacteria and virulence factors). Therefore, since PBL does not always involve active odontogenic infection, it is reasonable not to find a significant relationship between PBL (including its pattern and severity) and MSMT.
References
1. Butaric LN, Wadle M, Gascon J, Pediatric Imaging N, Study G. Anatomical variation in maxillary sinus ostium positioning: Implications for nasal-sinus disease. Anat Rec 2019;302:917-930
2. Shankar L. The Normal Anatomy of the Paranasal Sinuses as seen with Computed Tomography and Magnetic Resonance Imaging. In: Shankar L, Evans K, Hawke M, Stammberger H, eds. An Atlas of Imaging of the Paranasal Sinuses. Toronto: Imago Publishing Ltd, 1994:41-72
3. White SC, Heslop EW, Hollender LG, Mosier KM, Ruprecht A, Shrout MK. Parameters of radiologic care: An official American Academy of Oral and Maxillofacial Radiology report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2001;91:498-511
4. Ata-Ali J, Diago-Vilalta J-V, Melo M, Bagán L, Soldini M-C, Di-Nardo C, et al. What is the frequency of anatomical variations and pathological findings in maxillary sinuses among patients subjected to maxillofacial cone beam computed Tomography? A systematic review. Med Oral Patol Oral Cir Bucal 2017;22:e400
5. Lu Y, Liu Z, Zhang L, Zhou X, Zheng Q, Duan X, et al. Associations between MSMT and apical periodontitis using cone-beam computed tomography scanning: a retrospective study. J Endod 2012;38:1069-1074
6. Block MS, Dastoury K. Prevalence of sinus membrane thickening and association with unhealthy teeth: a retrospective review of 831 consecutive patients with 1,662 cone-beam scans. J Oral Maxillofac Surg 2014;72:2454-2460
7. Brüllmann DD, Schmidtmann I, Hornstein S, Schulze RK. Correlation of cone beam computed tomography (CBCT) findings in the maxillary sinus with dental diagnoses: a retrospective cross-sectional study. Clin Oral Investig 2012;16:1023-1029
8. Nunes CA, Guedes OA, Alencar AHG, Peters OA, Estrela CR, Estrela C. Evaluation of periapical lesions and their association with maxillary sinus abnormalities on cone-beam computed tomographic images. J Endod 2016;42:42-46
9. Raghav M, Karjodkar FR, Sontakke S, Sansare K. Prevalence of incidental maxillary sinus pathologies in dental patients on cone-beam computed tomographic images. Contemp Clin Dent 2014;5:361
10. Rege ICC, Sousa TO, Leles CR, Mendonça EF. Occurrence of maxillary sinus abnormalities detected by cone beam CT in asymptomatic patients. BMC Oral Health 2012;12:1-7
11. Smith KD, Edwards PC, Saini TS, Norton NS. The prevalence of concha bullosa and nasal septal deviation and their relationship to maxillary sinusitis by volumetric Tomography. Int J Dent 2010;2010:404982
12. Patel NA, Ferguson BJ. Odontogenic sinusitis: an ancient but under-appreciated cause of maxillary sinusitis. Curr Opin Otolaryngol Head Neck Surg 2012;20:24-28
13. White SC, Pharoah MJ. White and Pharoah’s oral radiology e-book: principles and interpretation. Elsevier Health Sciences,2018
14. Hoskison E, Daniel M, Rowson J, Jones N. Evidence of an increase in the incidence of odontogenic sinusitis over the last decade in the UK. J Laryngol Otol 2012;126:43-46
15. Brook I. Sinusitis of odontogenic origin. Otolaryngol Head Neck Surg 2006;135:349-355
16. Connor S, Chavda S, Pahor A. Computed tomography evidence of dental restoration as an aetiological factor for maxillary sinusitis. J Laryngol Otol 2000;114:510-513
17. Maillet M, Bowles WR, McClanahan SL, John MT, Ahmad M. Cone-beam computed tomography evaluation of maxillary sinusitis. J Endod 2011;37:753-757
18. Vallo J, Suominen-Taipale L, Huumonen S, Soikkonen K, Norblad A. Prevalence of mucosal abnormalities of the maxillary sinus and their relationship to dental disease in panoramic radiography: results from the Health 2000 Health Examination Survey. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010;109:e80-e7
19. Whyte A, Boeddinghaus R. The maxillary sinus: physiology, development and imaging anatomy. Dentomaxillofac Radiol 2019;48:20190205
20. Bayrak S, Ustaoglu G, Demiralp KO, Çakmak ESK. Evaluation of the characteristics and association between Schneiderian membrane thickness and nasal septum deviation. J Craniomaxillofac Surg 2018;29:683-687
21. Vidal F, Coutinho TM, Carvalho Ferreira Dd, Souza RCd, Gonçalves LS. Odontogenic sinusitis: a comprehensive review. Acta Odontol Scand 2017;75:623-633
22. Blickman JG, Parker BR, Barnes PD. Pediatric radiology: the requisites e-book. Elsevier Health Sciences, 2009
23. Capelli M, Gatti P. Radiological study of the maxillary sinus using CBCT: the relationship between mucosal thickening and common anatomic variants in chronic rhinosinusitis. J Clin Diagn Res 2016;10:MC07
24. Shanbhag S, Karnik P, Shirke P, Shanbhag V. Association between periapical lesions and MSMT: a retrospective cone-beam computed tomographic study. J Endod 2013;39:853-857
25. Nascimento EHL, Pontual MLA, Pontual AA, Freitas DQ, Perez DEC, Ramos-Perez FM. Association between odontogenic conditions and maxillary sinus disease: a cone-beam computed tomography study. J Endod 2016;42:1509-1515
26. Gomes AC, Nejaim Y, Silva AI, Haiter-Neto F, Cohenca N, Zaia AA, et al. Influence of endodontic treatment and coronal restoration on status of periapical tissues: a cone-beam computed tomographic study. J Endod 2015;41:1614-1618
27. Estrela C, Bueno MR, Azevedo BC, Azevedo JR, Pécora JD. A new periapical index based on cone beam computed Tomography. J Endod 2008;34:1325-1331
28. Gonzalez SM. Interpretation basics of cone beam computed Tomography. John Wiley & Sons, 2021.
29. Insua A, Monje A, Chan HL, Zimmo N, Shaikh L, Wang HL. Accuracy of Schneiderian membrane thickness: a cone-beam computed tomography analysis with histological validation. Clin Oral Implants Res 2017;28:654-661
30. Huang Y-T, Hu S-W, Huang J-Y, Chang Y-C. Assessment of the relationship between maxillary sinus membrane thickening and the adjacent teeth health by cone-beam computed tomography. J Dent Sci 2021;16:275-279
31. Phothikhun S, Suphanantachat S, Chuenchompoonut V, Nisapakultorn K. Cone-beam computed tomographic evidence of the association between PBL and mucosal thickening of the maxillary sinus. J Periodontol 2012;83:557-564
32. Sheikhi M, Pozve NJ, Khorrami L. Using cone beam computed Tomography to detect the relationship between the PBL and mucosal thickening of the maxillary sinus. J Dent Res 2014;11:495
33. Shahidi S, Zamiri B, Panahi R. Evaluation of the association of sinus mucosal thickening with dental and periodontal status using cone beam computed tomographic imaging. J Dentomaxillofac 2016;5:38-39
34. Kuan EC, Suh JD. Systemic and odontogenic etiologies in chronic rhinosinusitis. Otolaryngol Clin North Am 2017;50:95 111
35. Puglisi S, Privitera S, Maiolino L, Serra A, Garotta M, Blandino G, et al. Bacteriological findings and antimicrobial resistance in odontogenic and non-odontogenic chronic maxillary sinusitis. J Med Microbiol 2011;60:1353-1359
36. Saibene AM, Vassena C, Pipolo C, Trimboli M, De Vecchi E, Felisati G, et al., editors. Odontogenic and rhinogenic chronic sinusitis: a modern microbiological comparison. Int Forum Allergy Rhinol 2016;6:41-45
This article licensed under the Creative Commons Attribution 4.0 International License CC-BY 4.0., which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are properly credited.
